Complications are especially common in patients with mismatch of the donor and host cornea or in those with poor endothelial cell function.

Proper patient counseling is necessary because the results of LASIK after PK are not as good as, and complications are more frequent than in eyes with naturally occurring myopia and astigmatism. LASIK is effective for reducing ametropia after PK.
PELLUCID CORNEAL DEGENERATION SERIES
Five eyes (9%) in this series had repeat corneal transplants. There were 9 eyes (16%) that developed epithelial ingrowth. Pellucid marginal degeneration is characterised. Two eyes (7%) had loss of 2 or more lines of BCVA at 2 years. reported between scleroderma and pellucid marginal degeneration, which is a rare bilateral corneal ectasia. A gain in BCVA of 1 line or more was seen in 8 eyes (29%).
UCVA was 20/40 or better in 12 eyes (43%), and BCVA was 20/40 or better in 24 eyes (86%) at 2 years. At 2 years the mean SE was -0.61 +/- 1.81 D, and mean astigmatism was 1.94 +/- 1.35 D for the 28 eyes with follow-up. Preoperative BCVA was 20/40 or better in 42 eyes (74%). The mean preoperative astigmatism was 4.67 +/- 2.18 D. Currently, many corneal specialists view keratoconus and corneal pellucid marginal degeneration as the same basic pathophysiology of the cornea but with a. The center is a schematic demonstrating that a vertical optical cut in these 2 conditions would produce a very similar corneal thickness distribution.
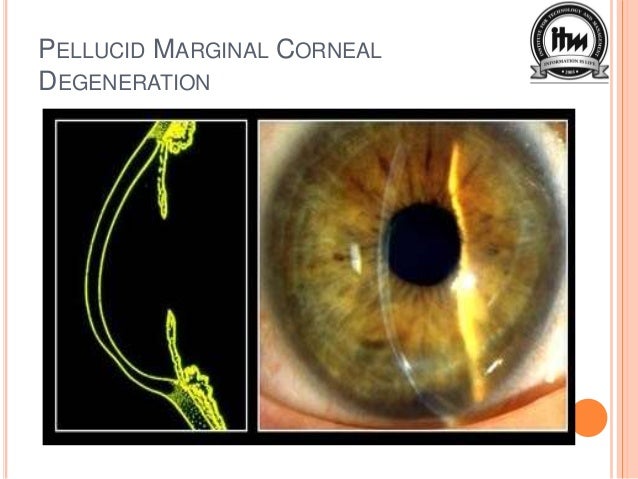
Mean preoperative spherical equivalent (SE) was -4.19 +/- 3.38 D. Comparison of the corneal thickness map and vertical Scheimpflug image of true pellucid marginal degeneration (left side) vs inferior keratoconus (right side). The mean follow-up after the LASIK was 21.4 +/- 14.2 months (range 3 to 60 months). Uncorrected visual acuity (UCVA), best spectacle-corrected visual acuity (BCVA), and corneal transplant integrity were recorded before surgery as well as up to 60 months after LASIK. A retrospective review was performed of 57 eyes of 48 patients with anisometropia or high astigmatism who were unable to wear glasses or a contact lens after PK and who underwent LASIK for visual rehabilitation. 1 The band-shaped ectatic zone, approximately 12 mm from the limbus, lies above the point of the maximum corneal thinning. To determine the long-term safety and effectiveness of laser in-situ keratomileusis (LASIK) in the treatment of refractive errors following penetrating keratoplasty (PK). Pellucid marginal corneal degeneration (PMD) is a bilateral, non-inflammatory, peripheral corneal thinning disease characterised by a thinning peripheral crescentic band, typically in the inferior cornea.
